了解診斷👩🏻🏫顯影技術,CT、MRI與PET有何不同🧐
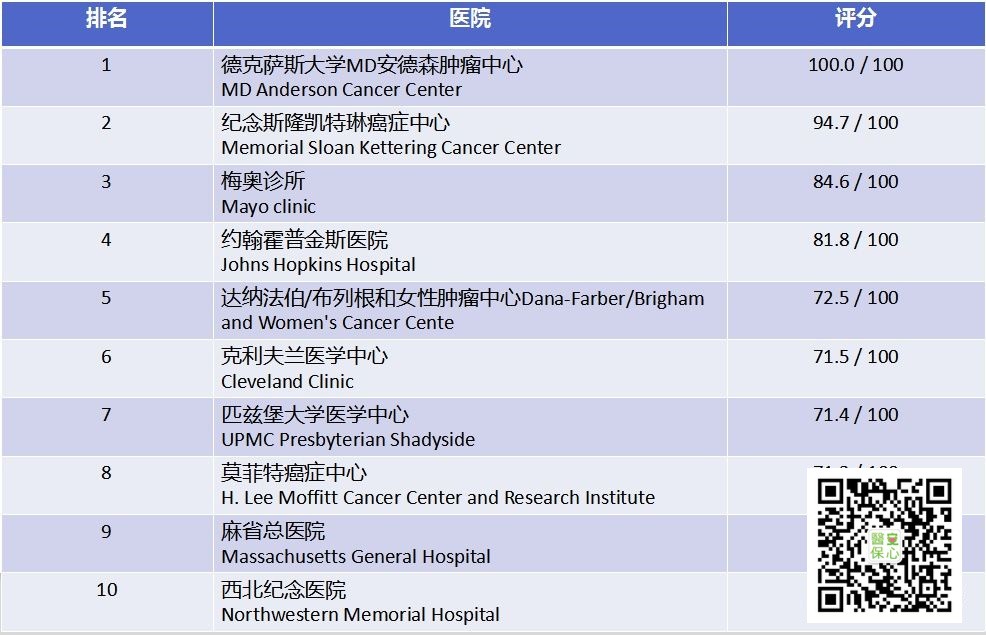
顯影技術,CT、MRI與PET有何不同? 當病人身上同一部位出現病徵,有的醫生建議做CT,有的醫生建議做MRI,讓病人感到困惑不解。然後又有些癌症病人要求做PET Scan,到底這些一個又一個的英文專業詞彙指的是什麼?它們又有什麼作用與分別? 什麼是CT? 電腦斷層掃描 (Computed Tomography,以下簡稱CT),是指利用無數的X光射線穿透人體。取得影像後,再由電腦予以組成二度空間影像,以觀察身體的內部。 「點看」美國最新癌症醫院排名 所以我們常聽到某某人做過多少切,看到幾條冠狀動脈阻塞,其實是指用X光來給器官做切片。切得越多片,影像就越清晰。然而我們不要盲目最求大數字,其實64切就已足夠。 CT有什麼優缺點? CT的優點是:快速、無痛,以及無需要求病患在掃描時保持靜止。缺點是:X光可能會致癌,不過單一檢查其輻射劑量並不會對人體造成危害;另外,所使用的顯影劑可能會傷腎,引發過敏反應等等。 什麼是MRI? 磁力共振成像 (Magnetic Resonance Imaging,以下簡稱 MRI),就是利用強大的磁場來引起原子核釋放電磁波,由於不同物質的氫原子含量不同,從而産生不同的共振現象,這種共振可被檢測並轉化為圖像。 而人體含有大量的氫原子,各器官和組織的氫原子含量差異很大,這種差異便是 MRI 診斷的基礎。 「點看」紐約特別救濟計劃-不影響移民身份的廉價醫療保險 MRI有什麼優缺點? 優點是無輻射及無痛。缺點是速度慢、噪音大,病患必須保持靜止,不可以有金屬物體(如心臟起搏器)等等。 到底CT與MRI有什麼分別?病患應如何選擇? MRI和CT都具有較高的軟組織分辨率,但MRI擁有更高的軟組織分辨率,且無骨性僞影。所以其優勢在於觀察顱腦、脊柱、關節、肌肉等病變,其中腦腫瘤、動脈瘤、椎間盤突出、半月板損傷等為首選。 而且MRI對腫瘤、血管和淋巴結之間的相互關係易於鑒別,故常可比 CT 更有效和更早期發現病變。而且 MRI 沒有X光幅射,是一種非常安全的檢查方法。 當然MRI也有其不足之處。首先是 MRI 掃描時間長,通常一個部位的掃描時間都超過 10分鐘,而 CT 大多僅需 10秒即可完成。 其次是 MRI 的空間分辨率明顯低於 CT,仍待進一步提高。再次,體內裝有心臟起搏器、鐵磁性金屬植入物等患者都不能進行 MRI 檢查。同樣基於 MRI 強大磁場限制, 很多生命支援儀器和搶救設備都不能進入 MRI 掃描室。 什麼是PET? 正電子掃描 (Positron Emission Tomography,簡稱PET Scan),則是核子醫學掃描檢查的一種。它利用一種相當先進的正電子掃描儀器進行全身或局部掃描檢查。近年,正電子掃描(PET Scan)在腫瘤治療方面扮演重要角色,是目前評估腫瘤最有效的檢查方法,能追蹤早期癌細胞病變,有助定位以便抽取癌細胞組織檢查,亦能偵測治療成效。 … Read more